Raising the Age of Eligibility for Medicare to 67: An Updated Estimate of the Budgetary Effects

CBO's new estimate of the net budgetary savings from adopting this policy is much lower than its earlier estimates for proposals to raise Medicare’s eligibility age. This report describes CBO’s new estimate and the reasons for the change.
Summary
Medicare, one of the federal government’s largest programs, provides health care benefits primarily to elderly people. The usual age of eligibility for those benefits is 65, although certain people qualify for the program earlier. (Medicare is available to people under age 65 who have been eligible for Social Security disability benefits for at least 24 months or who have end-stage renal disease.) Outlays for Medicare are projected to increase rapidly in coming decades because of the retirement of the baby-boom generation and because growth in per capita spending for health care is expected to continue to exceed growth in per capita gross domestic product over the long term. Moreover, increases in life expectancy mean that the average length of time that people are covered by Medicare has risen significantly since the program began in 1965. That trend, which increases the program’s costs, will almost certainly continue.
In the course of preparing its forthcoming report on options for reducing the budget deficit, the Congressional Budget Office (CBO) updated its analysis of an option to raise the eligibility age for Medicare from 65 to 67. The agency’s new estimate of the net budgetary savings from that option is much lower than its earlier estimates for proposals to raise Medicare’s eligibility age. This report describes CBO’s new estimate and the reasons for the change.
What Policy Option Did CBO Analyze?
The option that CBO analyzed would raise the age of eligibility for Medicare by two months every year, beginning with people who were born in 1951 (who will turn 65 in 2016), until the eligibility age reached 67 for people born in 1962 (who will turn 67 in 2029). Thereafter, the eligibility age would remain at 67. Those changes are similar to the ongoing increases in Social Security’s full retirement age (FRA)—the age at which workers become eligible for full retirement benefits—except that scheduled increases in the FRA include a 12-year period during which the FRA remains at 66. (Unlike Medicare, which has a single eligibility age, Social Security allows workers to receive reduced retirement benefits as early as age 62, and the majority of eligible people choose to claim Social Security benefits before reaching the FRA.) Under this option, the eligibility age for Medicare would remain below Social Security’s FRA until 2029, when both would be 67 for people born in 1962; from that point on, the two eligibility ages would be identical.
A change in the eligibility age for Medicare would affect people’s sources of health insurance coverage, including Medicaid. States have the option under current law to expand their Medicaid programs to people with income below 138 percent of the federal poverty guidelines. Although that optional Medicaid expansion applies only to people under age 65, for this option, CBO assumed that the age limit would increase in tandem with Medicare’s eligibility age.
What Is CBO's New Estimate?
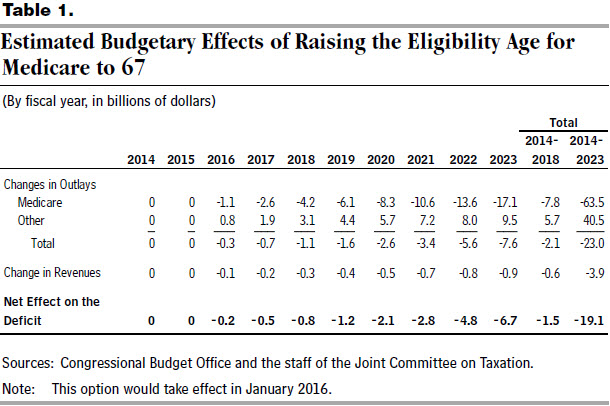
Implementing this option would reduce federal budget deficits by $19 billion between 2016 and 2023, according to estimates by CBO and the staff of the Joint Committee on Taxation (see Table 1). That figure represents the net effect of a $23 billion decrease in outlays and a $4 billion decrease in revenues over that period. The decrease in outlays includes a reduction in federal spending for Medicare as well as a slight reduction in outlays for Social Security retirement benefits. However, those savings would be substantially offset by increases in federal spending for Medicaid and for subsidies to purchase health insurance through the new insurance exchanges and by the decrease in revenues.
Outlays for Medicare would be lower under this option because fewer people would be eligible for the program than the number projected under current law. In addition, outlays for Social Security retirement benefits would decline slightly because raising the eligibility age for Medicare would induce some people to delay applying for retirement benefits. One reason is that some people apply for Social Security at the same time that they apply for Medicare; another reason is that this option would encourage some people to postpone retirement to maintain their employment-based health insurance coverage until they became eligible for Medicare. CBO expects that latter effect would be fairly small, however, because of two considerations: First, the proportion of people who currently leave the labor force at age 65 is only slightly larger than the proportion who leave at slightly younger or older ages, which suggests that maintaining employment-based coverage until the eligibility age for Medicare is not the determining factor in most people’s retirement decisions. Second, with the opening of the health insurance exchanges, workers who give up employment-based insurance by retiring will have access to an alternative source of coverage (and may qualify for subsidies if they are not eligible for Medicare). This option could also prompt more people to apply for Social Security disability benefits so they could qualify for Medicare before reaching the usual age of eligibility. However, in CBO’s view, that effect would be quite small, and it is not included in this estimate.
Other effects of this option would add to budget deficits, but by smaller amounts. Federal spending for Medicaid would increase for two groups of people whose age was between 65 and the new eligibility age for Medicare: those who, under current law, will be dual-eligible beneficiaries (Medicare beneficiaries who also qualify, on the basis of income and assets, to receive benefits from Medicaid) and those who will be beneficiaries of Medicaid before turning 65 and will lose that eligibility under current law once they qualify for Medicare. This option would cause Medicaid to remain the primary source of coverage for members of both groups until they reached the new eligibility age for Medicare.
Subsidies for health insurance coverage purchased through the exchanges would also increase under this option because some of the people whose eligibility for Medicare would be delayed would instead obtain insurance through the exchanges and would qualify for subsidies. (Those subsidies take two forms: tax credits to cover a portion of the premiums for policies bought through the exchanges and additional subsidies to reduce cost-sharing payments under those policies. The premium subsidies are structured as refundable tax credits, and CBO estimates that, in most cases, the amounts of those credits will exceed the total amount of federal income tax that recipients owe; the amounts that offset the taxes that recipients owe are classified as revenue losses, and the amounts that exceed the taxes owed are classified as outlays. Subsidies for the cost sharing of enrollees in exchange plans are also categorized as outlays.)
This option would also affect federal revenues, decreasing them by an estimated $4 billion between 2016 and 2023. That decline is the net result of several partly offsetting effects, the largest of which would be a reduction in federal revenues because of the increase in exchange subsidies. A small portion of those additional subsidies would take the form of reduced revenues rather than outlays, as discussed above.
Looking farther into the future, CBO estimates that by 2038, spending on Medicare would be about 3 percent less under this option than it would be under current law—4.7 percent of gross domestic product rather than 4.9 percent. On the basis of its estimates for 2016 through 2023, CBO projects that roughly two-thirds of those long-term savings from this option would be offset by the increases in federal spending for Medicaid and exchange subsidies and the reduction in revenues described above.
Although CBO anticipates that most people who would lose eligibility for Medicare under this option would continue their existing health insurance coverage or switch to other forms of coverage, the number of people without health insurance would increase slightly. For example, CBO estimates that of the 5.5 million people who would be affected by this option in 2023, about 50 percent would obtain insurance from their (or their spouse’s) employer or former employer, about 15 percent would continue to qualify for Medicare on the basis of their eligibility for disability benefits, about 15 percent would buy insurance through the exchanges or in the nongroup market, about 10 percent would receive coverage through Medicaid, and about 10 percent would become uninsured. To develop those estimates, CBO examined data on the patterns of health insurance coverage among people a few years younger than Medicare’s current eligibility age. CBO then adjusted those figures to account for changes in sources of health insurance coverage and in participation in the labor force as people age.
How Much Did CBO's Estimate Change and Why?
CBO’s current estimate of the savings to Medicare from this option is much lower than its earlier estimates for proposals to raise Medicare’s eligibility age. For example, in a report published in January 2012, CBO estimated that such a policy change would produce budgetary savings of $113 billion over 10 years.
The current, lower estimate primarily reflects a new assessment by CBO that some of the people whose eligibility for Medicare would be delayed under this option would not cost Medicare as much, under current law, as CBO previously projected. CBO’s current estimate incorporates a detailed analysis of the cost of 65- and 66-year-old Medicare beneficiaries.
CBO’s analysis highlighted two points. First, at ages 65 and 66, beneficiaries who enrolled in Medicare when they turned 65 tend to be in much better health—and thus are substantially less expensive, on average—than beneficiaries who were already enrolled upon turning 65 (because of disability or end-stage renal disease). Second, the many 65- and 66-year-old beneficiaries who are workers (or workers’ elderly spouses) with employment-based health insurance are less costly to Medicare, on average, than other beneficiaries at those ages. For most of those workers, employment-based health insurance is the primary source of coverage, and Medicare is a secondary payer—meaning that Medicare’s payments are limited to the cost-sharing obligations that beneficiaries face under their employment-based health insurance policies. Moreover, most beneficiaries for whom Medicare is a secondary payer wait to enroll in Parts B and D of Medicare until they (or their spouses) stop working. As a result, Medicare spends much less on Part A services for those beneficiaries than it does for beneficiaries for whom Medicare is the primary payer, and it does not pay for services covered under Parts B and D.
Taking into account both of those factors—differences in health status between beneficiaries who enroll in Medicare at age 65 and those already enrolled by 65, and the effect of secondary-payer status—caused a significant reduction in CBO’s estimate of Medicare spending under current law for beneficiaries who would be affected by the increase in the eligibility age. Mostly as a result of those changes, CBO’s current estimate of the net costs to Medicare of those beneficiaries under current law is roughly 60 percent lower than CBO’s previous estimates.
By contrast, CBO’s estimate of the extent to which this option would increase federal spending for Medicaid and exchange subsidies has not changed significantly. Compared with previous estimates, a similar proportion of beneficiaries who would lose Medicare eligibility under this option are estimated to enroll in Medicaid or the health insurance exchanges.
The much smaller reduction in Medicare spending, combined with a similar increase in non-Medicare spending, results in a net change in projected outlays that is much smaller than previously estimated. Additionally, CBO’s new estimate includes the option’s projected effects on federal revenues, which was not included in previous estimates.

